What is Psoriasis?
An autoimmune disease, psoriasis leads to acceleration in skin cell growth resulting in a buildup of dead skin cells as new skin cells grow under. This chronic disease results in white, scaly patches of skin that are dry and often inflamed.
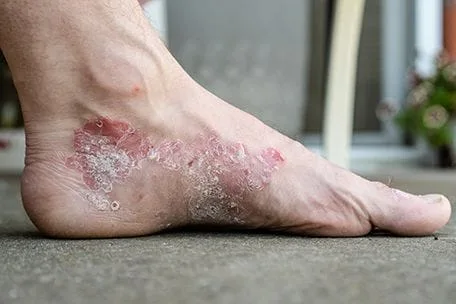
Patients diagnosed with psoriasis go through cycles of flare ups, which can occur for weeks or months at a time. Psoriasis occurs for each patient differently—some many only experience patches of psoriasis on their elbows and scalp, while others may develop psoriasis on the soles of their feet. This is known as plantar psoriasis.
What Are the Causes of Psoriasis?
According to the National Psoriasis Foundation, psoriasis is quite a common disease. It currently affects approximately 8 million people in the U.S. alone. Normal skin cell production averages a month from the development of new skin cells to the shedding of old ones.
However, for patients with psoriasis, this process is rapidly accelerated due to an overactive immune system. As a result, skin cell production takes only three to four days and instead of dead skin cells sloughing off, they pile up on the skin's surface, creating psoriasis plaques.
Common causes of psoriasis include:
- genetics
- stress
- certain infections such as strep throat
- use of certain types of medications—beta-blockers
- smoking
- excess alcohol intake
- weather—cold, drier climates can lead to more psoriasis flares
- allergies
- certain foods
What Are the Symptoms of Psoriasis?
Psoriasis may be mild for some, while others experience psoriatic plaques on different parts of the body. Common symptoms of psoriasis include:
- thick patches of silvery-white scaly skin that's red
- itchiness and burning
- dry skin, prone to bleeding
- white thickened nails on your feet
- small pus-filled sacs on the soles of your feet—for patients with pustular psoriasis
Some patients may also develop psoriatic arthritis, which causes inflammation of the joints, as well as stiffness and swelling.
What to Expect During Treatment for Psoriasis at the Podiatrist
If you're experiencing psoriasis on your feet, it's best to seek advice from a podiatrist on how to manage and treat psoriasis flares. Since psoriasis also produces similar symptoms to athlete's foot, a podiatric physician will be able to correctly diagnose and treat your condition.
A thorough foot examination, as well as a complete medical history, including your diet and lifestyle choices, are to be expected from your podiatric appointment. Fungal tests to rule out the presence of tenia pedis may also be given. Treatment depends on how severe the psoriasis symptoms are, and can include:
- topical medicines for mild to moderate psoriasis flare ups
- UV light therapy
- immunomodulatory drugs known as biologics—for patients with severe psoriasis who have not responded well to other treatment forms. These include Humira, Stelara, and Amevive
Learning what triggers your psoriasis is the best form of prevention since no cure currently exists for psoriasis. Avoiding alcohol and smoking, as well as certain types of foods and managing your levels of stress, can all help to reduce your psoriasis flare ups.
