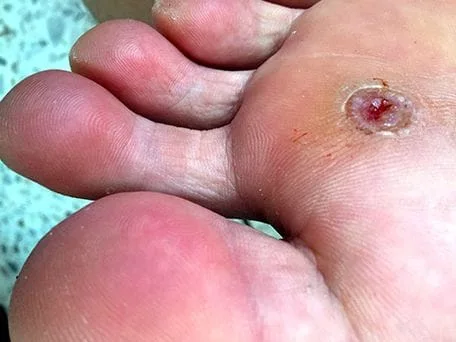
What is a Diabetic Foot Ulcer?
For patients with diabetes, proper foot care and regular checkups with your podiatrist are essential to preventing foot ulcers that may arise from a simple wound, cut, blister, or callus. They are open sores that are slow to heal and most commonly arise on the plantar surface of the feet of patients with diabetes.
Diabetic foot ulcers are one of several symptoms that patients with diabetes experience—in fact, studies show that the incidence of foot ulcers affects approximately 6% of patients in the US annually.
Diabetic foot ulcers are also the reason why amputation among patients with diabetes is high—they account for 84% of diabetes-related lower limb amputations.
What Are the Causes of Diabetic Foot Wounds?
The causes of diabetic foot ulcers include:
- peripheral neuropathy, resulting in damage of nerve endings in the foot
- peripheral artery disease causing lack of blood flow
- your ethnicity—Latinos, Asian Americans, African Americans, Pacific Islanders, and Indigenous Americans all have a higher risk of developing foot-related complications due to diabetes
- Charcot foot
- constant body weight on the feet
- patients with type 1 diabetes
- heart, kidney, and eye diseases caused by diabetes
Both lack of blood flow—also known as lower extremity ischemia—and damage to the nerve endings—due to high blood sugar levels over time—result in a greater incidence of foot ulcerations in patients with diabetes.
The inability to feel pain when a cut, scrape, or wound occurs on the lower legs or feet often leads to open sores that are slow to heal. The incidence of diabetic foot ulcers also increases with the age of a patient, as well as how long they've had diabetes.
What Are the Symptoms of Diabetic Foot Ulcerations?
As nerve and blood vessel damage is common in patients with diabetes, pain is not a common symptom of diabetic foot ulcers. The lack of a patient's ability to feel pain is one of the main reasons why cuts and blisters are left untreated for so long, leading to the formation of ulcers.
If you've had foot ulcers in the past or have recently been diagnosed with peripheral neuropathy, here are a few common symptoms to look out for:
- redness or swelling, especially on the bottom of the feet or the big toe area
- drainage on socks
- the appearance of calluses, corns, or blisters—if left untreated, these can lead to foot ulcers
- odor—often a symptom of a more severe ulcer
What to Expect During a Diabetic Wound Care Treatment
Daily foot care is essential to preventing the onset of foot ulcers in patients with diabetes. Checking your feet daily allows you to look out for scrapes, cuts, calluses, and blisters, which can be treated properly by your podiatric physician. The risk of diabetic foot ulcers increases if you:
- have peripheral neuropathy
- wear improper footwear
- have hammertoes, bunions, or bony protrusions
- drink alcohol
- high cholesterol levels
Immediate care should be sought out if an ulcer is present to improve a patient's overall level of wellness and reduce the risk of it worsening and amputation. If you've never been to a podiatrist before, you might wonder what to expect during your first appointment. First, your podiatric physician will begin with a comprehensive health history, including your current diet and lifestyle choices. From there, you may have a monofilament test done to determine if peripheral neuropathy affects one or both of your feet.
Treatment of diabetic foot ulcers by your podiatrist will involve:
- debridement—involves the removal of dead skin and necrotic tissue, if the ulcer is severe
- dressing the wound—to promote healing, also includes the use of medication
- off-loading—taking pressure off the ulcer through the use of orthotic walkers, custom-fit shoes, and boots
- treatment of an active infection with antibiotics
- control of blood glucose levels
- stem cell therapy
- hyperbaric oxygen therapy (HBO)
A less common form of treatment involves surgery. This may be done to:
- improve off-loading—excision or shaving of bone(s) in the feet
- correct foot deformities such as bunions and hammertoes
- treat infected bone
For more information about diabetes and its effect on feet, visit the American Diabetes Association.
